Clinical Solutions for Herniated Discs & Radiculopathy in the Roaring Fork Valley
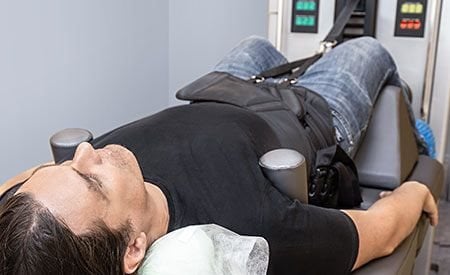
How Does the Roaring Fork Lifestyle Induce Disc Failure?
Biomechanics of Local Spinal Injuries
When I analyze spinal trauma at our clinic, the root cause rarely stems from a single event, but rather repetitive mechanical overload specific to our region's active lifestyle. The extreme sports and physical labor profiles in Basalt, Aspen, Carbondale, and Glenwood Springs create distinct patterns of spinal deterioration.
- The Arbaney Kittle Flexion Fault: Aggressive mountain biking on Arbaney Kittle Trail requires prolonged seated lumbar flexion combined with heavy shock absorption. This specific posture forces the nucleus pulposusposteriorly, stretching the annulus fibrosus until microscopic tearing occurs, ultimately leading to radiating nerve root irritation.
- The Aspen/Snowmass Rotational Torque: Mogul skiing and aggressive carving in Aspen/Snowmass generate immense shear forces through the lumbar and thoracic spine. These high-velocity rotational sports traumas easily overload the facet joints, leading to acute disc herniations and sudden sciatic nerve compression.
- Cervical Load from Remote Work: For our local professionals commuting down the valley, sustained desk work results in predictable, catastrophic postural shifts. We consistently observe severe hypertonicity of the pectoralis major and upper trapezius with reciprocal inhibition of the deep cervical flexors. This biomechanical collapse creates an anterior head carriage that exponentially multiplies the sheer weight on the lower cervical discs, inevitably triggering peripheral neuropathic numbness down the arms.
How Do We Heal Herniated Discs Without Surgery?
Our Targeted Modality Arsenal
When I treat a complex disc extrusion or radiculopathy, passive rest is not a solution. We actively stabilize the spinal column and stimulate deep tissue repair utilizing a highly specialized clinical toolkit. We never rely on outdated, painful stretching racks; instead, we target the exact neurological interference.
- Structural Repositioning: To physically open the intervertebral foramen and relieve the compressed nerve, we utilize biomechanically specific Gonstead pelvic alignments, Thompson drop-table protocols, and traditional Diversified techniques. For patients with high acute pain, we use the low-force Activator method to ensure safe joint mobilization. This approach is highly validated; independent peer-reviewed literature continually demonstrates the efficacy of spinal manipulation for lumbar radiculopathy.
- Cellular Regeneration: Once the joint is structurally stabilized, we address the damaged disc and surrounding inflamed tissues. We integrate photobiomodulation via Class IV Laser Therapy directly into the affected nerve roots. This drastically accelerates ATP production and reduces inflammation. Clinical studies support this exact mechanism, showing rapid cellular repair via low-level laser therapy for discogenic pain.
- Soft Tissue & Extremity Integration: A lumbar disc injury severely impacts your gait. We utilize Trigger Point Ultrasound and advanced soft tissue modalities to break up scar tissue in the compensating hip musculature, alongside targeted Extremity Adjusting to correct resulting ankle or knee imbalances.
Why We Recommend the Thompson Technique for Acute Discs Why do I specifically utilize the Thompson drop-table system for a patient walking in with a hot, acute lumbar herniation? Because the pneumatic drop mechanism allows us to deliver a precise, high-velocity, low-amplitude thrust that leverages the body's natural momentum. This minimizes the sheer force required to move the segment, bypassing the patient's protective muscle spasms, and safely gapping the facet joint to immediately pull pressure off the compromised nerve root.
Why Travel to Willits Town Center in Basalt for Spinal Rehabilitation?
Clinical Precision Over Generic Adjustments
When you are managing a compromised spinal cord or degenerating discs, proximity should not dictate your quality of care. Patients regularly commute from Aspen and Glenwood Springs to our clinic in Willits Town Center because we refuse to treat complex neuropathies with a generic five-minute "crack."
Frequently Asked Questions
How long does it take for a herniated disc to respond to targeted chiropractic care? While every disc pathology is unique, most patients notice a significant reduction in acute radicular pain within the first 4 to 6 sessions as we de-rotate the spine and apply laser therapy to reduce the localized chemical inflammation around the nerve root. Full structural stabilization requires ongoing, measured care.
Is it safe to get adjusted if I have active sciatica and leg numbness? Yes, but the technique matters. We do not use aggressive twisting motions on acute disc herniations. Instead, we utilize the Thompson drop-table or the low-force Activator method to gently gap the joint space and relieve the exact point of nerve compression without aggravating the surrounding protective muscle spasms.
Should I stop hiking or skiing during my treatment at Spine Spot Chiropractic? During the initial acute phase of your recovery, I will likely recommend modifying activities that introduce heavy rotational or sheer forces. However, our ultimate clinical goal is to rebuild your structural resilience so you can return to the mountains safely, rather than permanently restricting your lifestyle.
Dr. James Fraser | Doctor of Chiropractic Dr. Fraser holds dual licensure as a Doctor of Chiropractic and a Physiotherapist. As a proud Palmer College of Chiropractic alumni, he brings elite-level structural correction and advanced soft-tissue rehabilitation to the Roaring Fork Valley, bridging the gap between clinical biomechanics and active local lifestyles.
If you are experiencing severe spinal pain, do not wait for the symptoms to centralize. Click here to secure a complete neurological and structural evaluation at Spine Spot Chiropractic today.
✉️ Request Appointment | 📅 Book Online| 📞 Call (970) 924-1015 | 💬 Text (970) 924-1015



